How long during gestation are the gonads indifferent?
the first 5 weeks
When do the testes begin to develop? the ovaries?
The testes begin to develop at gestational weeks 6-7 while the ovaries begin to develop at week 9
What are the cell types of the male gonads?
germ cells, Sertoli cells, and Leydig cells
What are the cell types of the ovaries?
the germ cells (produce oogonia), granulosa cells, and theca cells
What structure gives rise to the epididymis, vas deferens, seminal vesicles, and ejaculatory ducts?
Wolffian ducts
What stimulates the growth and differentiation of the wolffian ducts?
testosterone. This testosterone from rach testis acts ipsilaterally (same side) on its own wolffian duct
T or F. Testosterone has to be converted to DHT to act on the wolffian ducts
F.
What causes atrophy of the mullerian ducts?
AMH from the Sertoli cells (this mullerian ducts would have become the female genital tract if they had not been suppressed by AMH)
When do the external male genitalia, the penis and scrotum, differentiate during gestation?
weeks 9-10
Growth and development of the external male gentialia depend on what?
covnersion of testosterone to DHT
Why do the mullerian ducts develop into the interal female tract (fallopain tubes, uterus, and the upper one third of the vagina) in women?
Because women lack AMH so the mullerian ducts develop by default
What happens if a gonadal female is exposed to high levels of androgens in utero (e.g. from excessive production by the adrenal cortex) when the external genitalia are differenitating?
a male phenotype will develop. If such exposure occurs AFTER differentiation of the external genitalia, the female phenotype is retained, but possibly with enlargement of the clitoris
In both males and females, gonadal function is driven by what?
the hypothalamic-pituitary axis
When does secretion of GnRH begin during gestation?
gestational week 4, but its levels remain low until puberty
When does secretion of LH and FSH begin during gestation?
between gestational weeks 10-12 (these too remain low until puberty)
T or F. During childhood, FSH levels are relatively higher than LH levels
T.
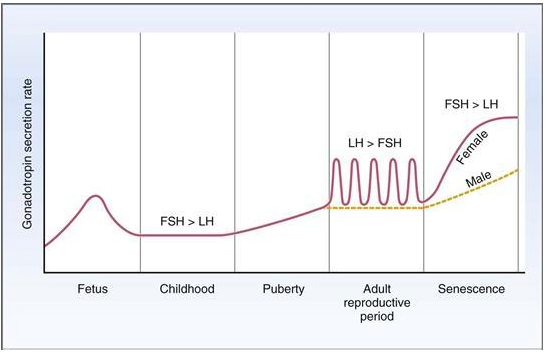
What happens to the secretion of GnRH, FSH, and LH after puberty?
it increases and becomes pulsatile, with the relative rates of LH becoming higher than FSH levels and the establishment of a 28-day cycle of gonadotropin secretion called the menstrual cycle
What happens to levels of GnRH, FSH, and LH in senescence?
gonadotropin levels increase further, with FSH levels becoming higher tahn LH levels again
What is one of the earliest events of puberty?
the appearance of large nocturnal pulses of LH during REM sleep and an increased sensitivity of the GnRH receptor in the anterior pituitary (thus, at puberty GnRH up-regulates its own receptor in the anterior pituitary and a given conc of GnRH produces a greater stimulation of FSH and LH secretion).
Pulsatile secretion of FSH and LH at puberty then stimulate what?
secretion of the gonadal steroid hormones, testosterone and estradiol, which then drive appearance of the secondary sex characteristics
T or F. The onset of maturational processes in men and women are genetic and programmed
T. For example, the age at menarche is similar between mothers and daughters (however, the mechanisms underlying the onset of pulsatile GnRH secretion remains a mystery)
What are the suggested thoughts on what causes the pulsatile increase of GnRH at puberty?
-Melatonin could inhibit GnRH (melatonin is high during childhood and decreases during adolescence, and removal of the pineal gland has been shown to precipitate early puberty)
Is the pulsatile nature of GnRH required to produce puberty and secondary growth or can the same effects be seen if you just give a long acting GnRH analogue?
It’s required! Puberty will NOT be initiated using a long-acting GnRH analogue in a GnRH deficient person



