Hair - too much or too little Flashcards
(65 cards)
What are the 3 types of hair?
- Lanugo hairs - soft hairs of the foetus. Shed by 4 months.
- Vellus hairs are fine, soft, non-pigmented hairs usually found covering the apparently hairless areas of the body.
- Terminal hairs are coarser, longer, pigmented hairs making up the eyebrows, eyelashes, scalp hair, pubic and axillary hair in men and women and much of the body and facial hair in men.
What are the 3 phases of hair growth?
- Anagen - active growth phase. 90% of hairs are in this.
- Catagen - Involutional stage.
- Telogen - resting and shedding phase. 5-8% of hairs.
How long does the anagen phase last on the scalp compared to the body?
2-6 years on the scalp
3-6 months on the body
How long does the catogen phase last on the body and scalp?
2-3 weeks
How long does the telogen phase last on the body and scalp?
3-4 month
What is the major class of hormone that affects hair growth?
What other hormones affect it?
Androgens
Thyroid. & Growth Hormone.
Why do androgens cause less hair on the scalp and more on the body?
Scalp anagen phase is less
Body anagen phase is more.
5a-reductase (converting testosterone to DHT) alters skin sensitivity & androgen receptors.
If many follicles go into the telogen phase at the same time, what is this called?
Telogen Effluvium
What are the 3 hair types?
- Nonsexual - grows independently of steroid hormones - eyebrows, forearms, lower legs.
- Ambosexual: dependent on female sex hormones (pubic triangle)
- Male sexual hair: androgen dependent-beard, nasal tip, ears.
Describe the hair cycle

What does an anagen hair look like under dermatoscope?
It has a sock.

if an anagen hair is pulled from the scalp, what does this mean?
It is pathological.
Look for a cause.
If a patient comes in with hairloss, What are some important questions to ask?
- Is it sudden or gradual?
- Sudden = telogen effluviu or Alopecia areata
- Gradual = pattern hair loss, CCCA
- Is the scalp itchy?
- Common in scarring alopecias
- Not common in non-scarring alopecias - tinea capitis.
- Do you eat meat?
- Low ferritin can cauise alopecia
- Do you menstruate regularly
- PCOS can cause increased androgen.
- Do both parents and siblings have a normal head of hair?
- Alopecia Areata runs in families.
- Medications - some Rx can cause hair loss.
- What styling processes or colouring do they use?
- Afro-hair is susceptible to heat and chemical straightening.
Describe the pull test
- 50-60 hairs are pulled gently between thumbs and fingers.
- Do this in multiple locations.
- Discard broken hairs.
-
Count the number of hairs:
- If 2 or less hairs - negative
- If 3 or more - positive - consider telogen or anagen effluvium.
- if 3 or more in one location - consider alopecia areata.
Describe the Bulging Hypothesis
- Stem cells are in the bulge area.
- These stems cells regenerate hair follicles, sebaceous glands and epidermis.

What are the causes of non-scarring alopecia?
- Alopecia Areata
- Androgenetic alopecia
- Telogen effluvium
- Anagen effluvium
- Tinea capitis
- Traumatic alopecia
What other autoimmune conditions is Alopecia Areata (AA) associated with?
- Vitiligo
- Psoriasis
- Thyroid disease
What signs or conditions are associated with worse outcome in AA?
- Nail pitting
- Pre-puberty onset
- Other autoimmune conditions.
What vitamin is often low in patients with AA?
Vitamin D
What kind of hair is pathognomonic for AA?
Exclamation Mark Hair

What can patients with AA complain about before AA becomes apparent?
Buzzing or tingling in hair
What 2 particular types of AA have a bad prognosis?
Atop associated AA
Ophiasis (baldness at the occiput of the scalp - see photo)
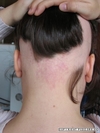
What is the best treatment for Alopecia Areata?
There is no proven single effective treatment.
- Under 5 years - no treatment
- 5-10 year - minoxidil 5% BD plus elocon
-
Over 10 years:
- Less than 50% involvement
- Triamcinolone 2.5% with Minoxidil 5% BD, Dermovate.
- Can try dithranol 1% for 1 hour plus 5% minoxidil BD.
- Over 50% - use of wigs.
- Less than 50% involvement
For patients with less than 50% hair loss, what can you use?
- Topical/Intralesional Steroids
- 5mg/ml of Triamcinolone for scalp
- 2.5mg.ml for eyebrows and beard areas.
- Every 6 weeks.
- Ensure EMLA cream on eyebrows.


















