What paperwork needs to be signed and witnessed before a client leaves for surgery?
Informed consent: surgery is an invasive procedure and there are risks the client needs to be aware of.
How to handle the informed consent:
- the HCP explains the risks
- the client signs the form and the nurse can sign as a witness
- if the client doesn’t understand the procedure or risks, the nurse informs the HCP
If it’s an emergency, the informed consent does NOT need to be signed.
What are the general nursing interventions before a client goes to surgery?
- all paperwork is completed
- labs have been obtained
- blood type and crossmatch in case of hemorrhage
- basic assessment and vital signs are obtained
- teaching on what to expect afterward has started
What clinical paperwork should be completed pre-operatively?
- history and physical: the HCP’s assessment of the client
- labs: check for abnormalities and report them to HCP
- diagnostic tests: specific to the problem
What are the nursing interventions after a client returns from surgery?
- assess for complications
- implement safety precautions
- teach about tubes, incisions, and preventing complications
What diet is the client on before surgery?
The client is NPO for at least 8 hours before surgery.
If it’s an emergency, the client can go to surgery right away.
NPO = nothing by mouth.
Which 2 bracelets should be applied to the client before surgery?
- ID bracelet with name, birthday, and medical record number
- medication allergy bracelet
What should be removed before the client goes to surgery?
Jewelry, makeup, dentures, hairpins, nail polish, glasses, contacts, and prostheses.
Where should the client’s valuables be placed in a healthcare facility?
Give valuables to family or lock in a safe.
What should be documented about the client pre-operatively in regards to going to the bathroom and medications?
- the last time the client ate, drank and urinated
- what meds were taken that day
What medication is commonly prescribed before surgery?
Antibiotics: to help decrease the risk of post-op infection
Pre-operatively, how will a client’s urinary needs be taken care of?
The client will either urinate before surgery or get a foley catheter inserted before surgery.

How will a surgical site be cleaned?
The site may be shaved and an antibacterial solution will be applied to prevent infection.
What psychological problem should be assessed before a client goes to surgery?
Assess for anxiety before surgery.
Give anxiolytic meds to decrease anxiety if needed.
If the client is having abdominal surgery, what treatment will the client get before the surgery?
The client may get an enema or laxative to clean out the bowels.
Teaching:
Pain control after surgery
- pain medicine options
- possible pain pump and how to use (patient-controlled analgesia/PCA)
- splinting the incision when coughing
Teaching:
Preventing pneumonia and atelectasis after surgery
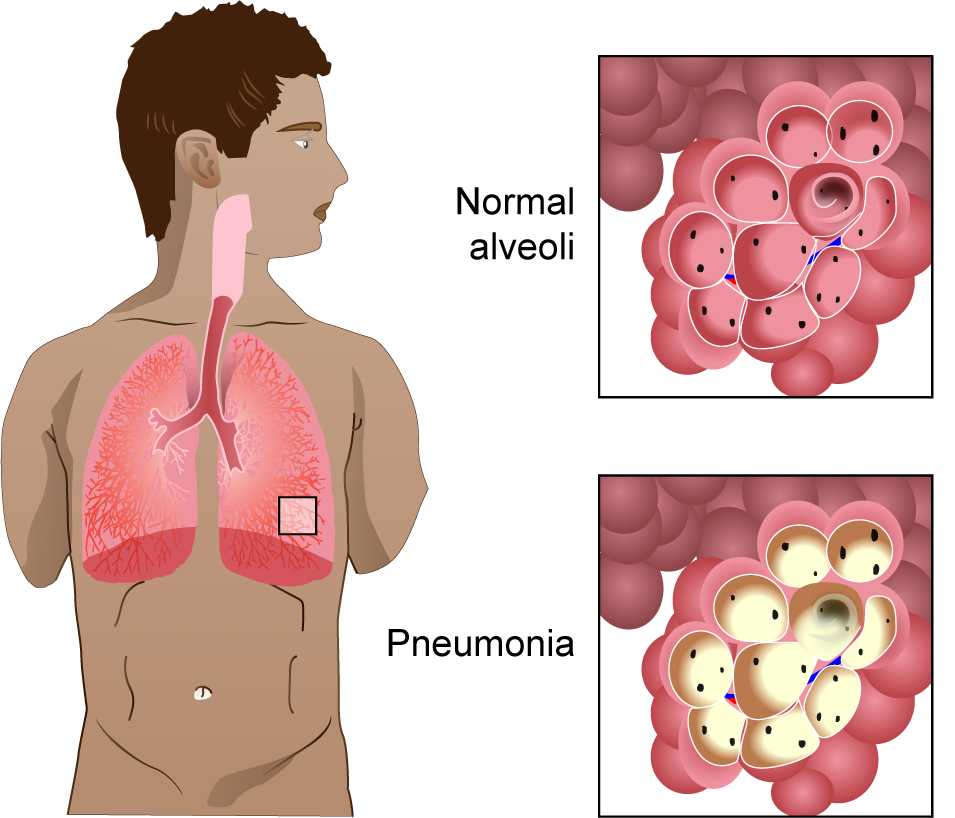
- turn, cough and deep breath
- use the incentive spirometer

Both of these interventions help open up the lungs and break up any mucus that may start to form.
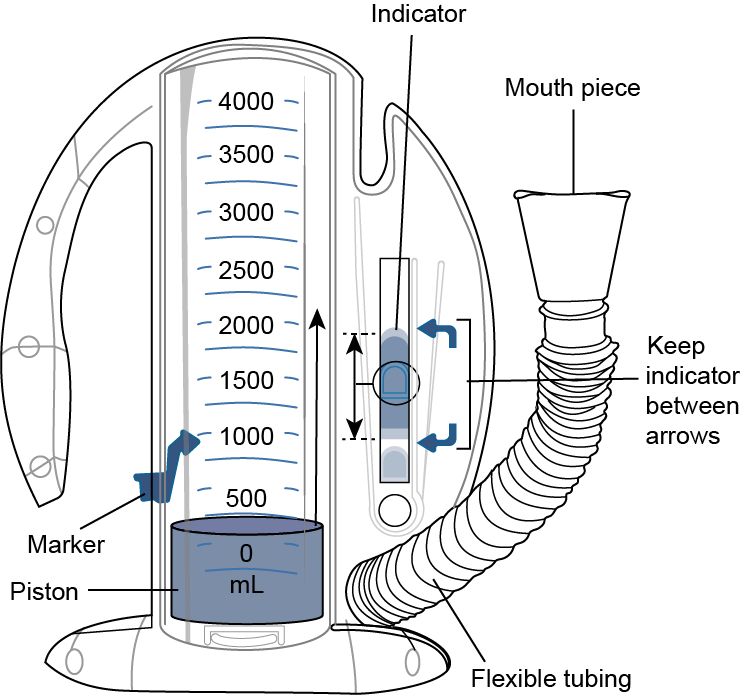
What are the 4 steps to teach the client about how to use an incentive spirometer?
- place mouth tightly around the mouthpiece
- inhale slowly and keep the floating indicator between 600 and 900 marks on the device (or higher marks depending on what the client can do)
- hold the breath for 5 seconds
- exhale through pursed lips
Repeat 10 times every hour!
Teaching:
Preventing deep vein thrombosis (DVT) after surgery
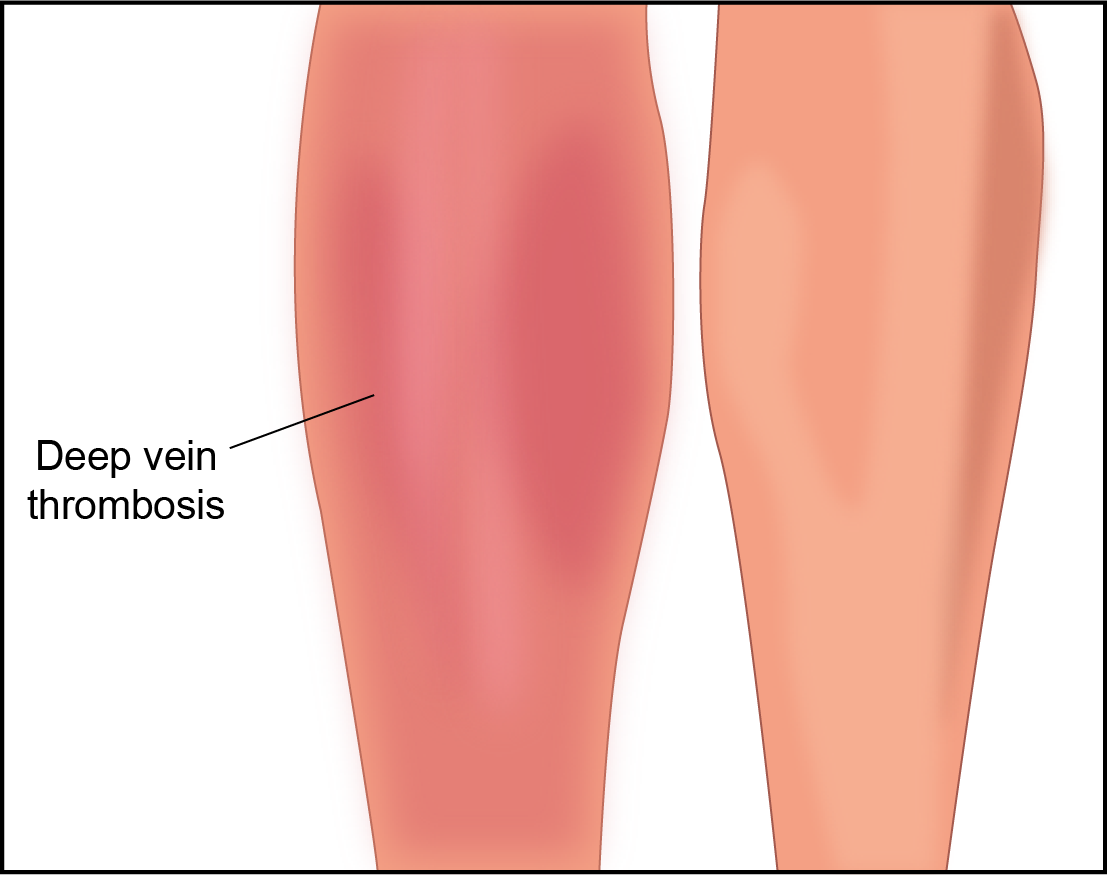
- ankle pumps/ foot exercises
- sequential compression devices (SCD boots)
- compression socks

These interventions increase blood circulation so the client doesn’t get a blood clot. If a blood clot forms it could break loose and travel to the lungs causing a pulmonary embolism that can kill the client.
Why is a set of vital signs obtained right before the client gets wheeled off for surgery?
To make sure the client isn’t having any obvious complications such as dysrhythmias, difficulty breathing, infection or bleeding.
Teaching:
Tubes and surgery
Inform where the tubes will be coming from so the client is not alarmed when waking up from surgery.
What are the common types of tubes or lines post-op?
- intravenous (IV) tubing
- Foley catheter
- wound drainage tubes (JP drain)
- chest tubes
- endotracheal tube (ET)
- nasal cannula
- nasogastric tube (NG)
- pulse oximeter (O2 sat)
- Telemetry (ECG or EKG)
- vacuum-assisted wound closure (wound vac)
What is this?

Foley catheter
What is this?
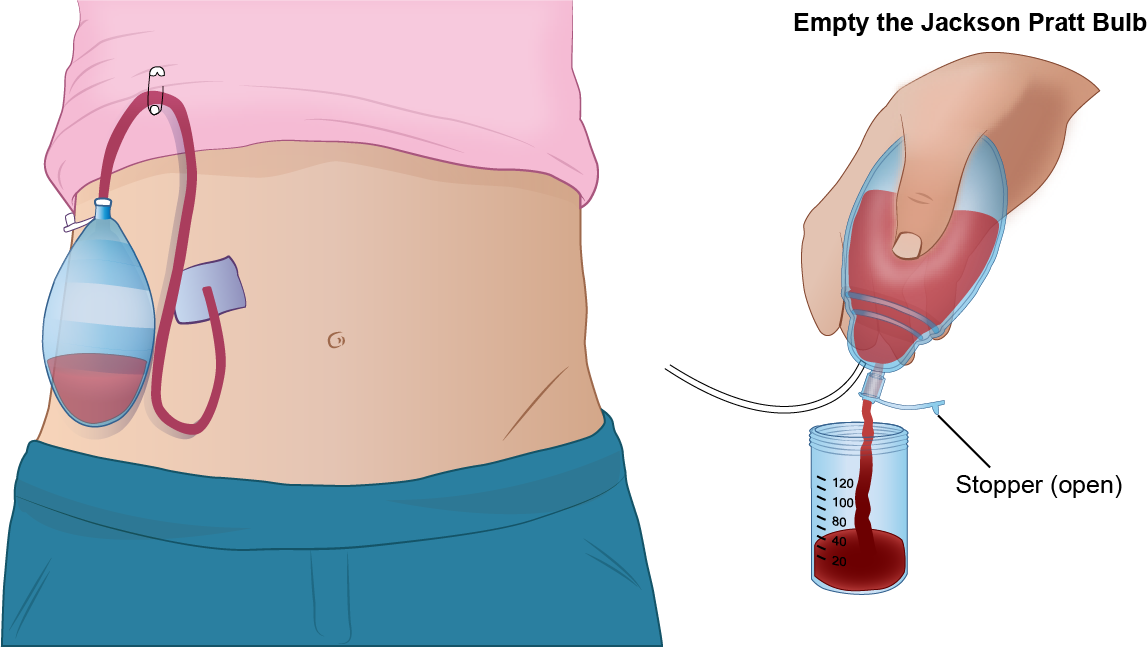
Wound drainage tube (Jackson-Pratt drain)
What is this?
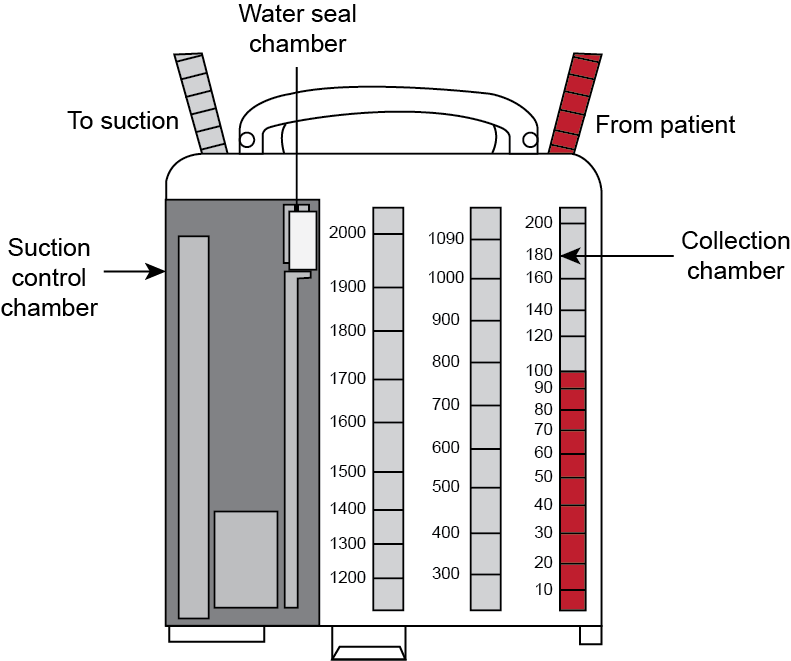
Chest tube container













