COPD
obstructive lung disease resulting from cigarette smoking and other toxic chemicals
airflow limitation that is not fully reversible, usually progressive and associated with an abnormal inflammatory response of the lung to noxious particles or gases
third leading cause of death in adults in the US, increasing in prevalence
causal risk factors of COPD
cigarette smoking
occupational exposures
genetic risk (alpha-1-antitrypsin deficiency)
genetic factors that predispose COPD
alpha-1-antitrypsin deficiency - PiZZ or PiMZ + smoking
single nucleotide polymorphisms - Type IV collagen alpha3, solute carrier familly 11 member 1 (SLC11A1), interleukin-1B
MMP-9 and CCL-1 increase severity and exacerbation risk
alpha-1-antitrypsin deficiency
coded by single gene on chromosome 14
PiZZ patients are severely deficient
PiSZ, Pi null-null, and Pi null-Z are also deficient
normal phenotyp eis PiMM
cigarette smoking is the most important risk factor
increased risk of cirrhosis and lung cancer as well
mechanisms of airflow obstruction in COPD
1) loss of tethering of airways due to emphysema - alveolar destruction resulting in decreased elastic recoil and airway collapse
2) remodeling of the small airways which causes plugging
3) increased mucous secretion which decreases the internal airway caliber and increases
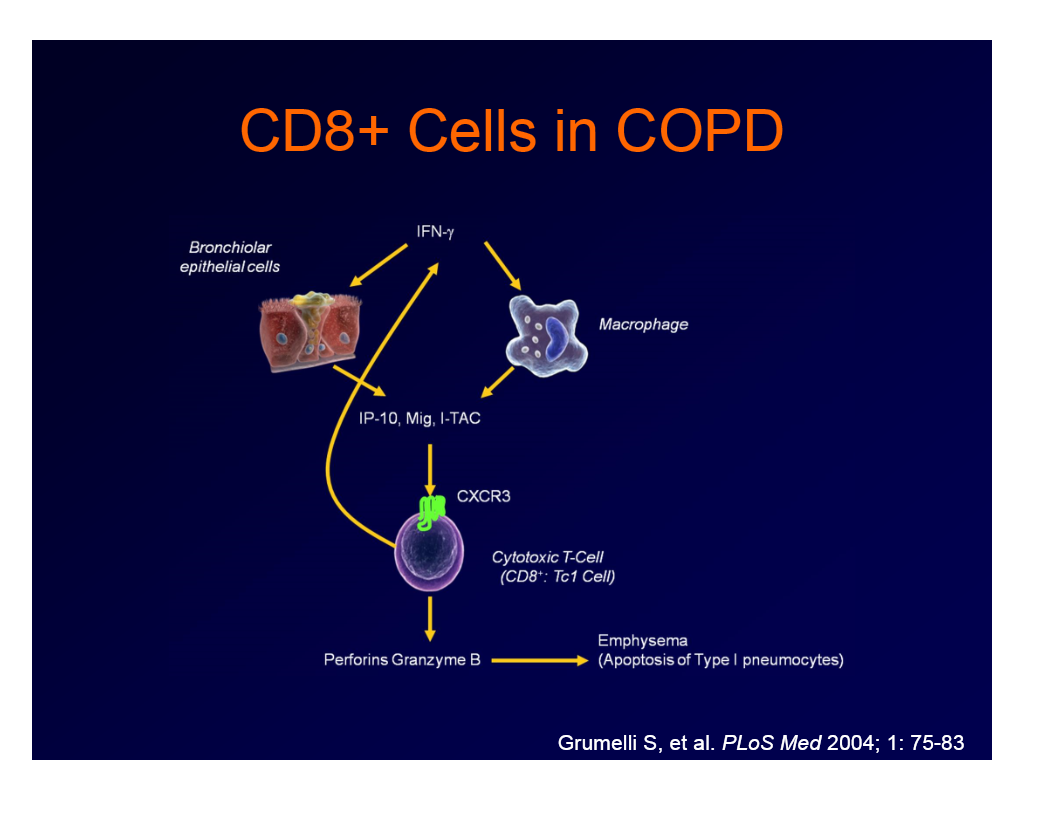
inflammatory cells involved in COPD
epithelial cells and alveolar macrophages activate fibroblasts,CD8+ lymphocytes, neutrophils, and monoytes
COPD is a nuetrophilic disease
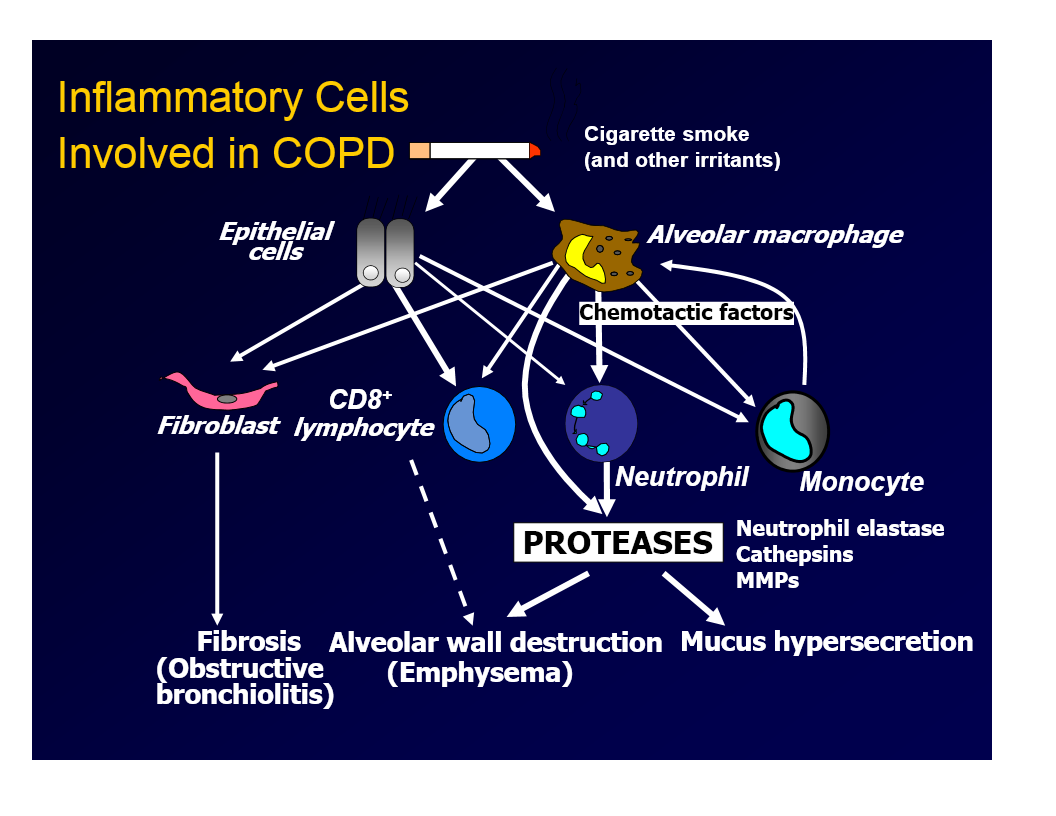
alveolar macrophages in COPD
orchestrate much of the inflammatory process
release mediators that attract neutrophils, monocytes, and CD8+ lymphocytes
release elastolytic enzymes and generate ROS
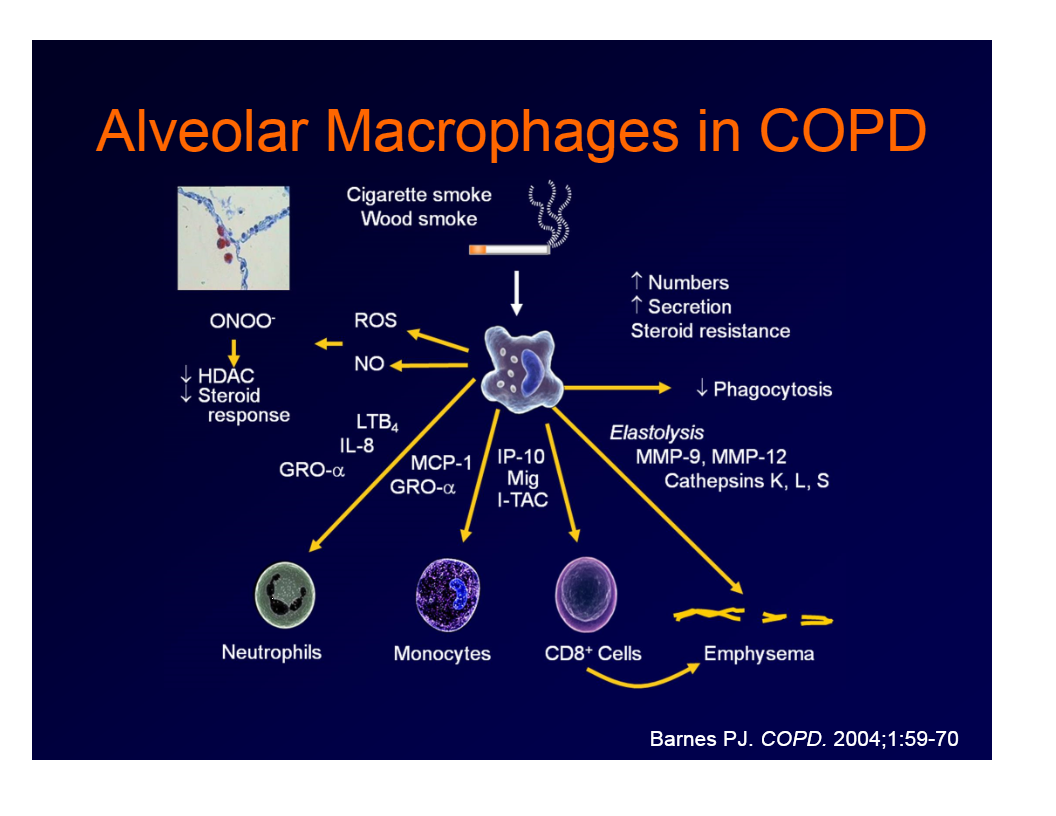
neutrophils in COPD
attracted by IL-8, LTB4 from macrophages and PMNs
release ROS and MPO which contribute to ongoing inflammatory response
serine proteases lik eneutrophil elastase contribute to destruction of th elung parenchyma
increased numbers of sputum neutrophils are associated with declining lung function
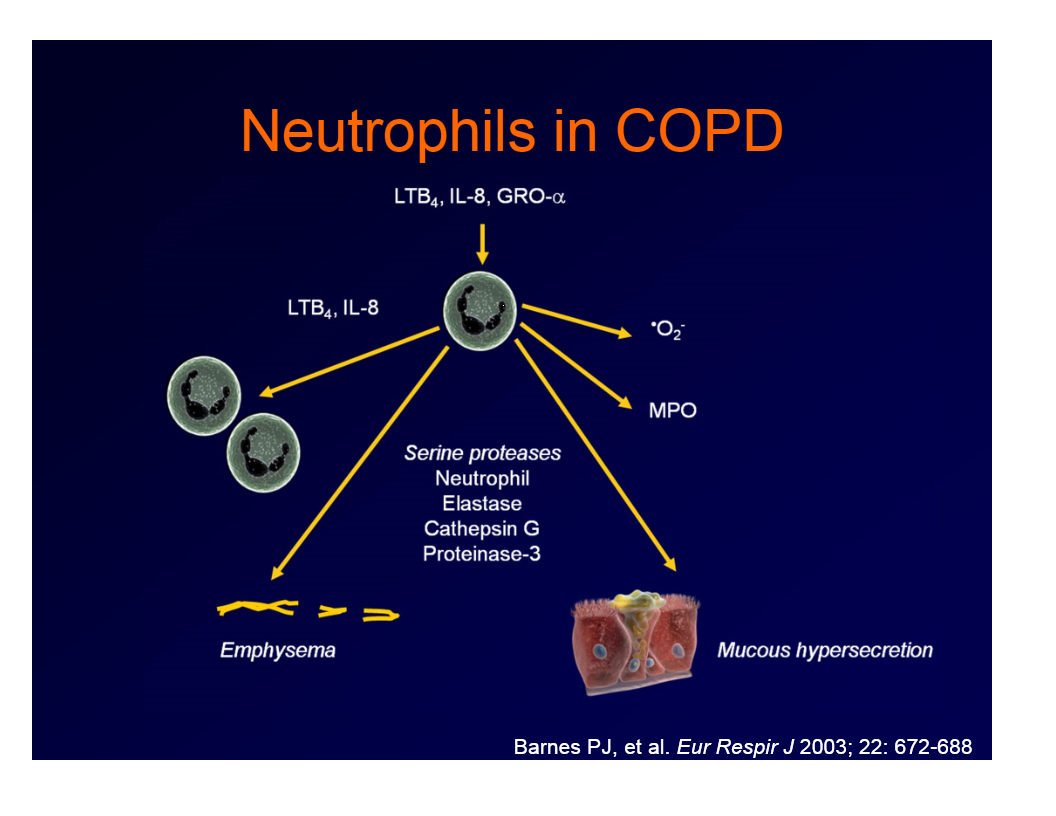
CD8+ lymphocytes in COPD
found in the airway walls, vessels, and lymph nodes of smokers with COPD
increased number associated with worse lung function
suggest that an antigenic process in the lung leads to abnormal inflammatory responses
perpetuate the inflammatory response by releasing chemoattractants
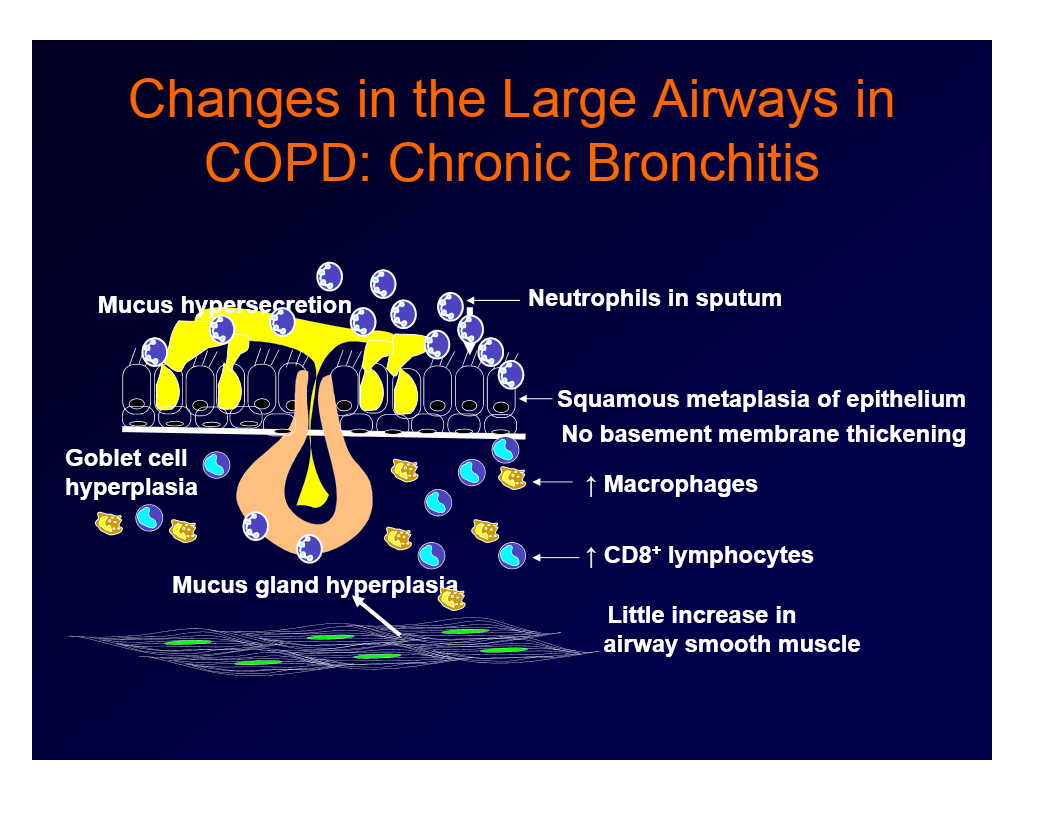
changes in the large airways in COPD
leads to chronic bronchitis
neutrophils in sputum
squamous metaplasia of epithelium, no basement membrane thickening
increased macrophages
increased CD8+ lymphocytes
mucous gland hyperplasia
goblet cell hyperplasia
mucous hypersecretion
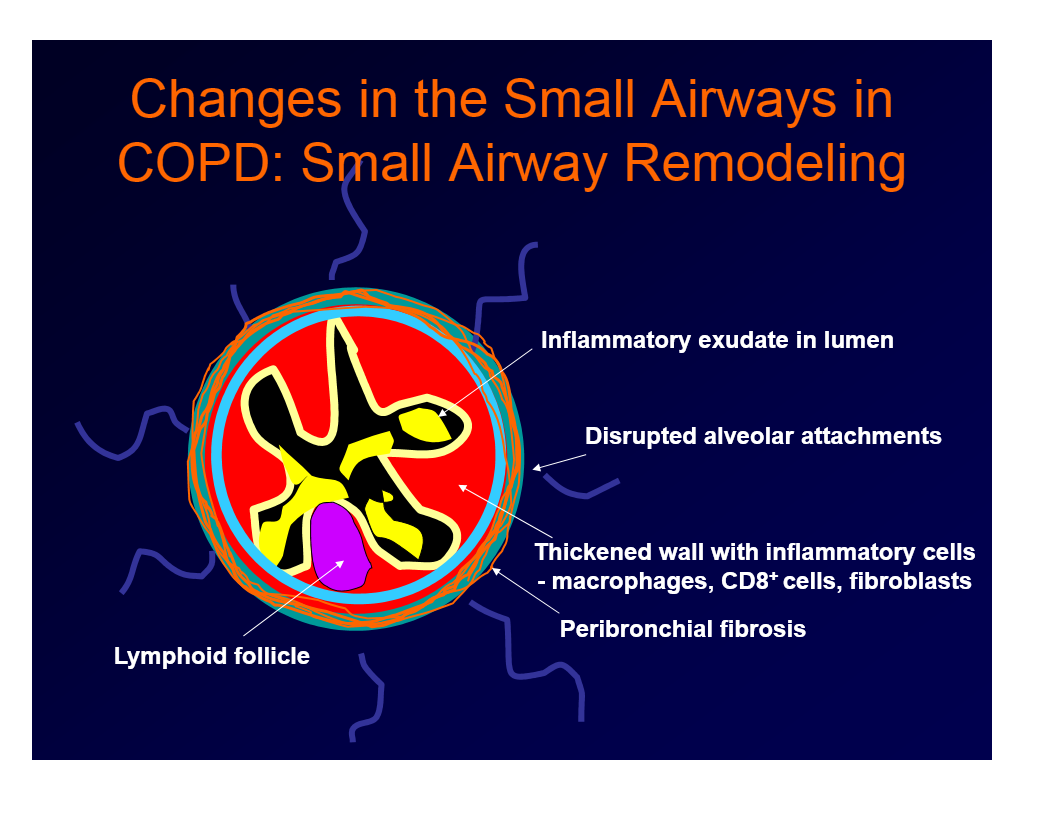
changes in the small airways in COPD
remodeling of the airways
inflammatory exudate in lumen
disrupted alveolar attachments
thcikened wall with inflammatory cells - macrophages, CD8+ cells, fibroblasts
peribronchial fibrosis
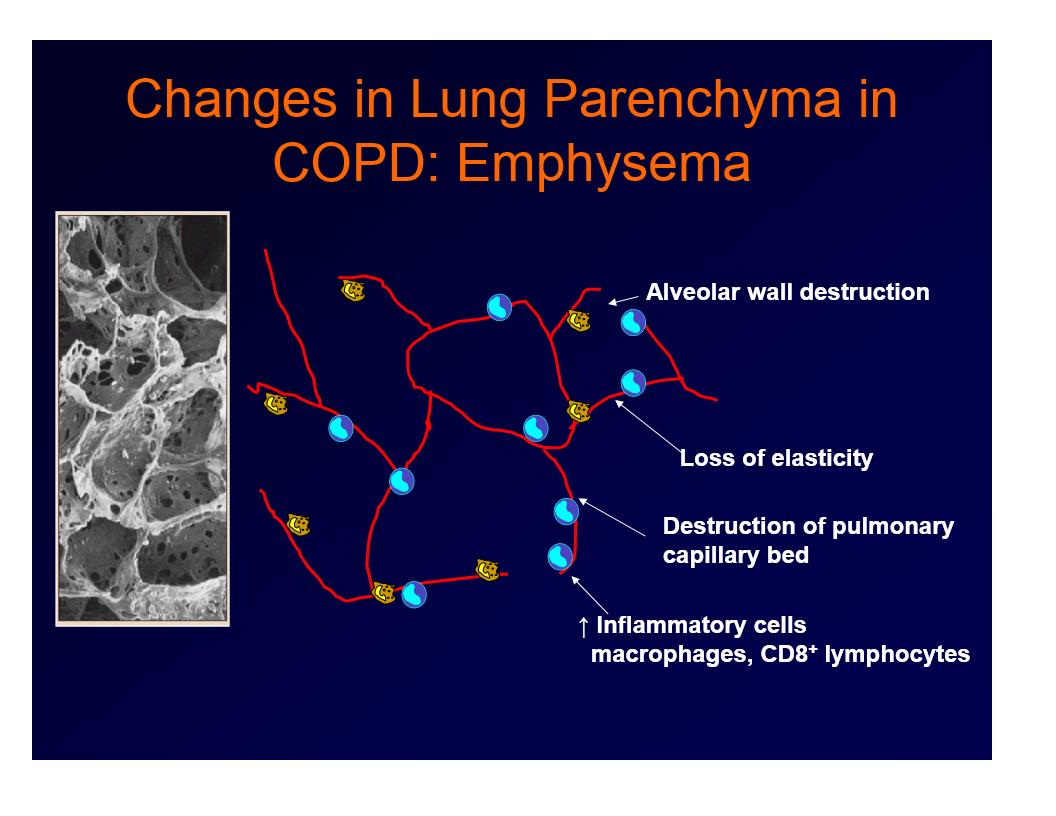
changes in lung parenchyma in COPD
emphysema
alveolar wall destruction
loss of elasticity
destruction of pulmonary capillary bed
increased number of inflammatory cells - macrophages, CD8+ lymphocytes
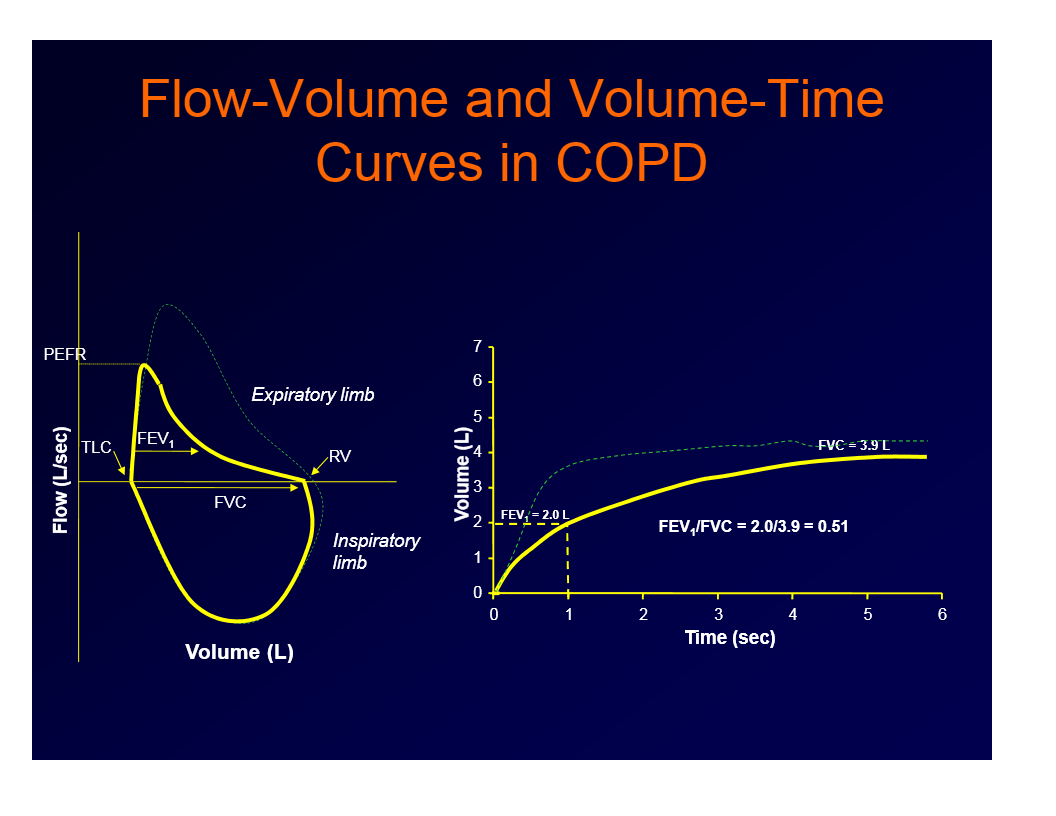
Describe the flow-volume and volume-time cirves in COPD.
flow-volume curve more concave, can’t reach the same peak outflow
volume-time curve flatter and takes longer to get closer to FVC
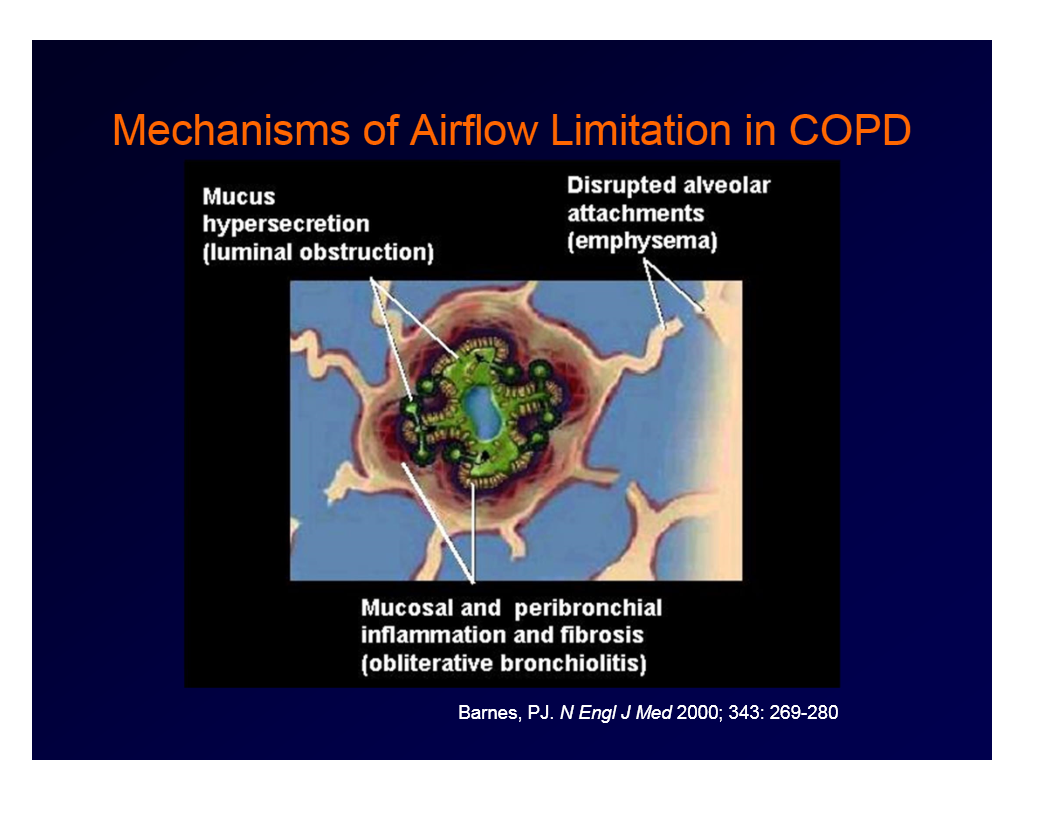
Mechanisms of Airflow Limitation in COPD
mucus hypersecretion (luminal obstruction)
disrupted alveolar attachments (emphysema)
mucosal and peribronchial inflammation and fibrosis (obliterative bronchiolitis
GOLD classification of mild COPD
FEV1/FVC < 70%
FEV1 >/= 80% predicted
GOLD classification of moderate COPD
FEV1/FVC < 70%
FEV1 between 50% and 80%<!--= FEV1 < 80% predicted</p-->
GOLD classification of severe COPD
FEV1/FVC < 70%
between 50% and 30% <!--= FEV1 < 50% predicted</p-->
GOLD classification of very severe COPD
FEV1/FVC < 70%
FEV1 < 30% predicted
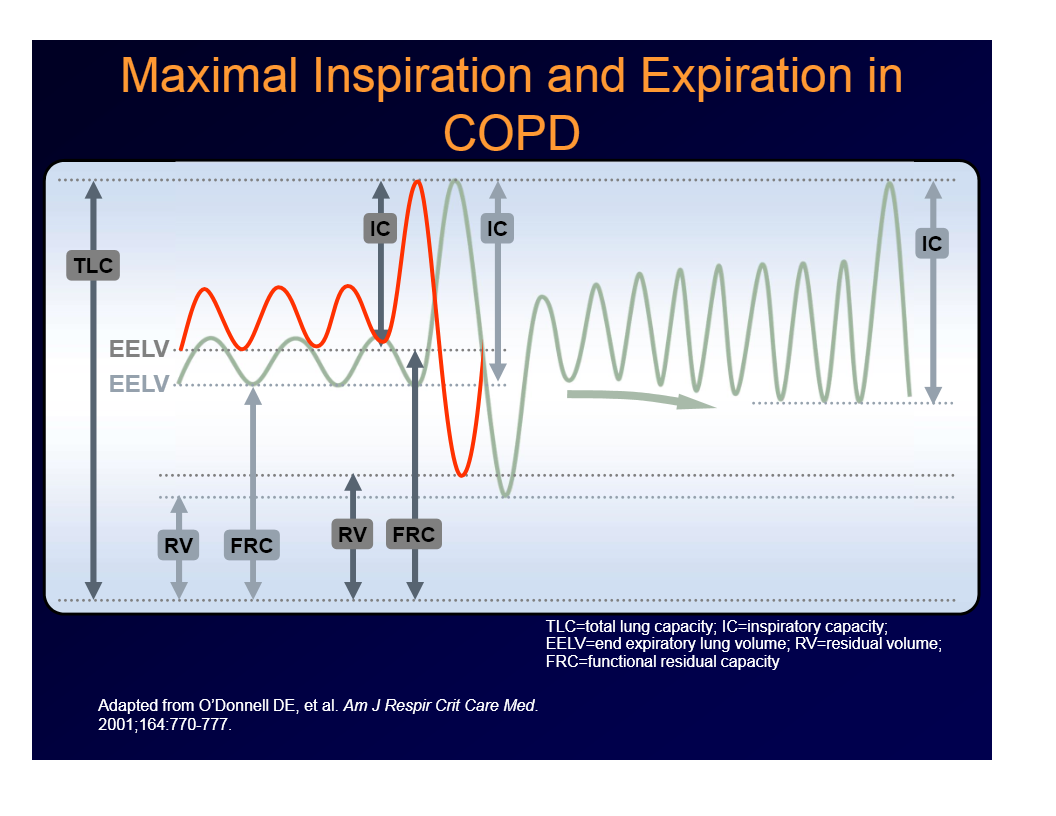
maximal inspiration and expiration in COPD
IC is decreased, RV is increased, FRC is increased
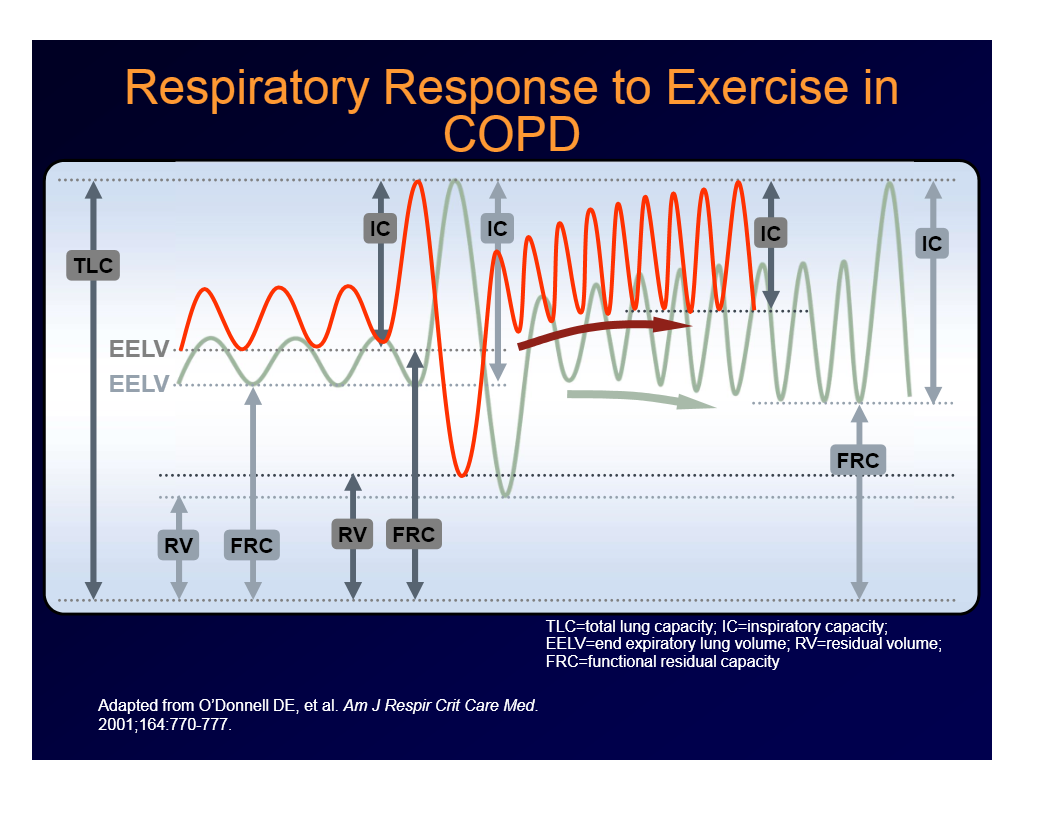
respiratory response to exercise in COPD
Lungs stay overinflated, more volume and less inspiration each breath
Can breath up to TLC, everything is shifted upward, IC is smaller
RR goes up
EELV goes up, dynamic lung hyperinflation, IC goes down
grade 0 mMRC dyspnea
breathless with strenuous exercise
grade 1 mMRC dyspnea
short of breath when hurrying onf the level or walking up a slight hill
grade 2 mMRC dyspnea
walk slower than people of the same age level because of breathlessness
have to stop for breath when walking at my own pace on the level
grade 3 mMRC dyspnea
stop for breath after walking about 100 meters of after a few minutes on the level


