Clostridum are gram _____ and ____ forming
positive and spore forming
Clostrium form _____ rods
anaerobic - they do not need oxygen to grow
________ imparts resistance to the drying heat, irradiation and disinfectants
endospore
Clostridium can survive for _____ in the environment due to the endospore
years
Clostridium is catalase _____, oxidase ______ and _______ ferments
negative, negative, they DO ferment
Clostrial cultures emit _____
putrid odor
CLostrium are motile via _____ flagella
peritrichous
(C. perferingens is non motile)
True/False: All clostridium produce endopores
False: Most Clostridium do not produce endospores
What Clostridium species is most common in humans and animals?
Clostridium perfringens
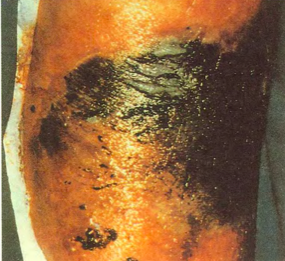
Clostridium is associated with enterotoxemias in ruminants, diarrhea, and wound infections that can lead to _____
gas gangrene (type A toxin)
Clostridium perfringens happens on farms with high diets of ______
carbohydrates
What are the virulence factors of Clostridium Perfringens?
adhesiosn- helps to bind to epithelial cells
capsule
Global regulatory systems - regulate toxin expression
Normally clostridium perfringens are present in the _____ or in the ______ of animals
intestinal tract or in the muscle
Bacteria moves into the muscle if there is muscle damage
When Clostridium Perfringens are in an environment that is not good for them they turn the regulatory system ____, but when the bacteria are in favorable conditions, the VirR and VirS start regulation the toxin production
off
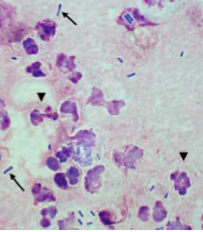
What would you see if you took a fine needle aspirate of an abscess with Clostridium?
Neutrophils that have been damaged or are in the process of dying. Along with Gram positive straight rods
_____ toxin is produced by all Clostridum perfringens and causes hemolysis, necrosis and lethality
alpha
_____ toxin is a pore forming toxin that is favored by protease inhibitors in colostrum
beta
______ toxin is activated by trypsin and is necrotizing and lethal to epithelial cells
Epsilon
Epsilon toxin concentrates in the brain and kidney and also damages the ______
microvasculature
_____ toxin affects the cellular cytoskeleton and kills the affected cell
Iota
________ (theta toxin) produces holes in the cellular membrane and is important for escape from the phagolysosome
Perfringolysin O
______ is produced by some C. perfringens during sporulation results in electrolyte abnormalities and diarrhea
Enterotoxin
What is the reservoir for Clostridium perfringens and how is it transmitted?
Intestinal tract and soil
it is transmitted via wound infection and ingestion
In the pathology of wound infection, what is the most important toxin and what does it cause?
alpha
causes cellulitis and gas gangrene (myonecrosis)