Path Lab-Female Repro Flashcards
(63 cards)
A 44 year old woman complains of persistent itching of the vulva. Creams recommended by her pharmacist provided no relief. Healthy since her last pregnancy more than 15 years ago, not seen by a gynecologist since then. Patient does not drink or smoke. Slightly overweight female. Vital signs normal. Examination of the vulva shows multiple white verrucous patches surrounding the introitus. CBC within normal range. Urinalysis negative for protein or glucose. Where are warty lesions from HPV 6 and 11 typically found?
HPV typically affects the vulva, vagina and cervix. The oropharynx and perianal region can also be involved. Note that 90% of vulvar intraepithelial neoplasia cases are due to HPV, especially HPV 16. Other causes include HSV-2.
35 year old woman was referred for follow-up secondary to findings of cytologic atypia in repeated PAP smears. She reports no other health problems and is employed in a business office. Patient enjoys the Friday bar scene. Had numerous “unfaithful” boyfriends. Her hobby is scuba diving and she travels 2-3 times per year for short vacations in the Caribbean. CBC within normal range. Urinalysis negative for protein or glucose. Biopsy showed a low-grade intraepithelial squamous cell dysplasia. How does this get to squamous cell carcinoma? What is her prognosis?
Progression from low grade must go through high grade before it can become full carcinoma. Spontaneous regression occurs in a majority of low grade lesions (most often associated with productive viral infections that are self limited) and a minority of high grade lesions.
A 33-year-old female complains of increasing pain during menstruation. Menarche at age 12. She stopped using oral contraceptives years ago and has regular menstruation. The patient and her husband would like to start a family, but she has never become pregnant. Occasional dysuria and dyspareunia. The patient is slender. Bimanual examination discloses enlargement of the left ovary with a possible cyst. Anterior tenderness is noted during the rectal exam. Biopsy is shown below. What is likely causing her condition? What finding is required to make the diagnosis of endometriosis?

Retrograde menstruation can cause endometriosis. Histologically you must see ectopic endometrial glands and stroma that are located outside of the uterus. Hemosiderin and fibrosis also found often.

A 34 year old woman complains of excessive fatigue. She has not seen her gynecologist for 7 years. She has two daughters ages 5 and 7. Her last pregnancy was difficult and she experienced excessive post-partum bleeding. The patient appears tired and pale. Her pulse is 92. The pelvic exam reveals nodular uterine enlargement. HCT 28 with MCV 68. Ultrasound consistent with submucosal and intramural tumors of the uterus. What is likely causing her condition?
Leiomyomas. These are found in premenopausal women and are estrogen sensitive. Extended menses occur due to poor uterine contraction and account for her microcytic iron deficiency anemia.
A 60-year-old female presents with vaginal bleeding. She has been taking conjugated estrogen medication for osteoporosis for the past 8 years. An endometrial biopsy performed 6 years ago showed endometrial hyperplasia. At that time she failed to return for follow-up. What is the most likely cause of her condition?
Endometrial carcinoma is the most common invasive cancer in the female genital tract, with high incidence in post-menopausal women. She has already been diagnosed with endometrial hyperplasia, which is a risk factor.
If you have HPV in the setting of a condyloma and a squamous cell carcinoma, which condition presents as shown below?

Koilocytic change represents an active HPV viral infection within the cells. Note the perinuclear halo and enlarged, hyperchromatic nuclei.
Why does cervical cancer tend to arise in the transition zone?

It tends to infect immature squamous cells which are found in the zone of transformation.

Which part of this pap smear is abnormal?

The clumps of cells are endocervical cells that are normal, the large cells are exocervical squamous cells. Abnormal cells are shown below with an enlarged nucleus and clumpy chromatin.

How do you know where to biopsy on culposcopy?
Acid staining of the cervix

What defines low grade squamous intraepithelial lesions?
Lack of maturation in the lower third of the mucosa. Note the amount of black in the cells indicating lots of viral protein and active infection.

What defines high grade squamous intraepithelial lesions?
Lack of maturation in the upper third of the mucosa.

What would you expect histology of this lesion to look like?

This is an exophytic squamous cell carcinoma

Why is cervical carcinoma worse than vulvar or vaginal carcinoma?

There is easier spread into local organs (ureter, bladder) and can lead to obstruction of the urinary tract.
A 44-year old woman complains of fullness after meals with vague lower abdominal discomfort. She had an appendectomy at age 17. Routine PAP smears have been consistently negative. She married at age 38 and has not been able to conceive. A maternal aunt died of breast cancer. No specific GI symptoms. She has been urinating with increased frequency. The abdomen is slightly protuberant. A mass is palpated in the right pelvis. Mild microcytic hypochromic anemia. WBC and differential normal. Urinalysis neg. Ultrasound demonstrates complex bilateral cystic masses in the lower abdomen. At surgical debulking prior to chemotherapy both ovaries are enlarged with cystic and solid masses. Cancer had extended to the pelvic organs, omentum, small bowel and liver surfaces (Stage III). What is the likely diagnosis and what are risk factors for this condition?
Serous cystadenocarcinoma. Abdominal discomfort is a common presenting factor in women with ovarian neoplasms. Age 45-65 is at highest risk for malignant ovarian tumors. Appendectomy rules out appendicitis and pseudomyxoma peritonei. FH of BRCA 1/2 mutations put her at risk for high grade serous carcinomas in the ovary. Nulliparity is also a risk factor. Of all the malignant ovarian tumors these are the most common. A significant portion of these cancers present bilaterally,
4 types of ovarian neoplasms
Surface epithelium (most common), germ cell, stromal and metastatic tumors.

Types of surface epithelial ovarian neoplasms
Serous, mucinous, endometriod (includes clear cell) and Brenner (composed of urothelium)

Type of germ cell ovarian neoplasms
Teratoma (most common germ cell) and dysgerminomas

Type of sex cord-stromal ovarian neoplasms
Granulosa-theca, sertoli and Leydig tumors.

Are most ovarian neoplasms functional or non-functional?
Most are non-functional. This means that they present as a mass that presents late and have a high mortality rate.
What would you expect this papillary ovarian neoplasm to look like on histology?
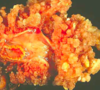
Papillary ovarian neoplasms tend to be benign. Below is a benign serous epithelial neoplasm of the ovary. Note that the proportion of epithelium to stroma is LOW w/minimal amount of epithelial proliferation around the stroma. Also note that there are no solid areas of epithelial growth and structures surrounded by epithelium are very simple. Note that in the lower image there is much more robust

What 3 conditions share molecular abnormalities that can arise in the uterus and ovaries?
Endometriosis, endometrial carcinoma and endometriod epithelial ovarian cancer.
Ovarian surface epithelial tumors that can be classified as benign, borderline and malignant?
Serous and mucinous cystadenomas.
How do you differentiate a serous from a mucinous cystadenoma in the ovary?
Most mucinous tumors are benign or borderline, serous are much more likely to be malignant. Serous tend to have bilaterally. Mucinous tend to be unilateral. Mucinous tumors tend to be larger and have a multilocular appearance.
How do you tell a mucinous from a serous cystadenoma of the ovary on histology?
Mucinous has tall